Pressure Ulcer Staging and Documentation
Pressure ulcer staging and documentation are imperative in all types of acute care settings and long-term care settings. If the nurse is able to document and assess everything they need, it makes your chances of winning a client’s case that much greater.
So what are pressure ulcers? Simply put, pressure ulcers (decubitus ulcers or bed sores), are injuries that break down the skin and underlying tissue. They are caused when an area of the skin is placed under immense pressure. They can range in severity from patches of discolored skin to open wounds that reveal bones and muscles. Today, we’re going to be discussing the importance of staging and documentation for these maladies, and how our LNC’s with SPLNC & Associates, LLC will help you come out with a legal victory.
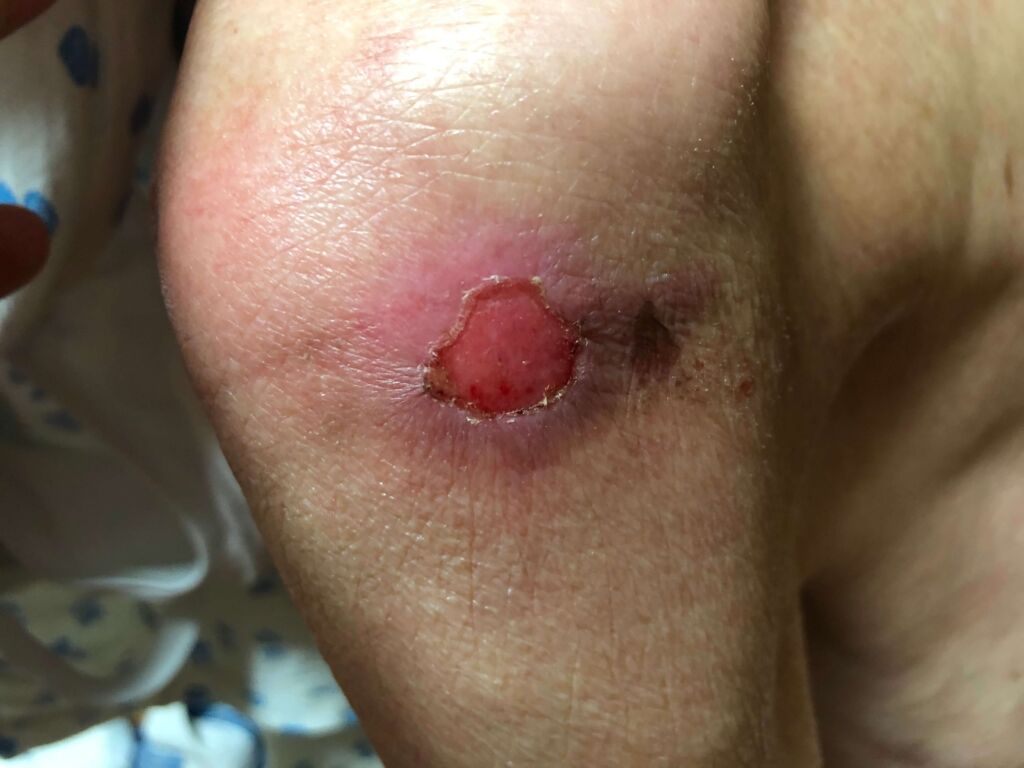
The Assessment and Staging Process
Once a pressure ulcer has been identified, it’s important that the correct stage of pressure ulcer is documented and assigned. The NPUAP (National Pressure Ulcer Advisory Panel) categories and stages are intended for describing pressure ulcers and not other skin ailments. The staging system is based on the type of tissue impacted or seen in the wound bed, as opposed to the depth of the wound in centimeters.
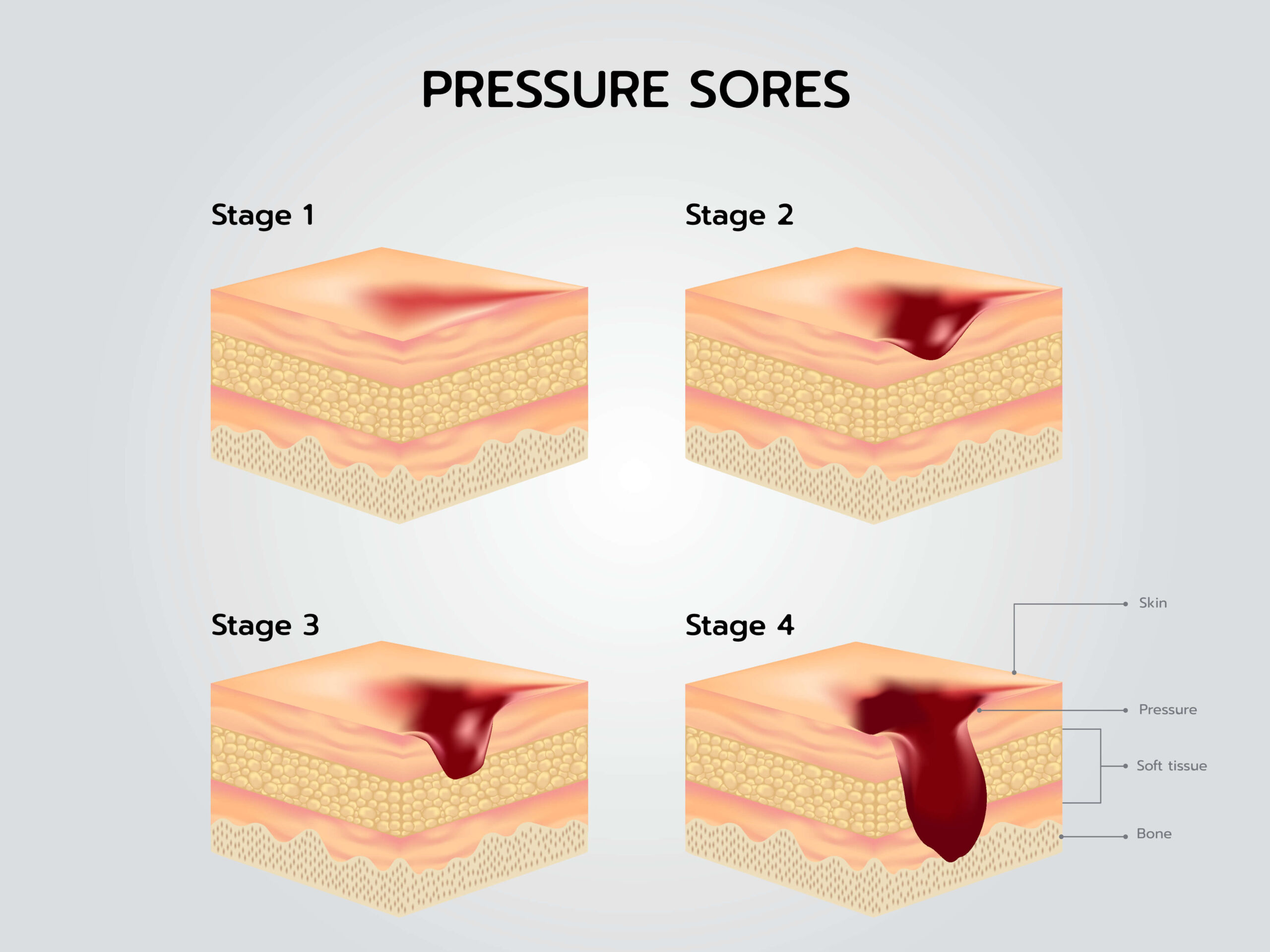
Here is a breakdown of the various stages:
- Stage I: A stage I pressure ulcer has redness on the surface of the skin. The NPUAP considers these stages as superficial injuries or wounds. When pressure/shear forces lead to non-blanchable erythema of intact skin over a bony prominence, the appropriate designation will always be stage 1.
- Stage II: A stage II classification is assigned when the epidermis is no longer intact, and the pressure-related erosion or ulcer is shallow, with no slough on the wound bed. These ulcers can also appear as an open or ruptured blister, including wounds in patients dealing with herpes, burns, or epidermolysis. The blister and etiology must be appropriately evaluated before pressure ulcer staging and documentation can occur.
- Stage III: In Stage III, injuries are sustained in the subcutaneous tissue (located below the dermis), but not through the underlying structures. Pressure ulcers in stage III have full-thickness tissue loss, but are differentiated when joint, muscle, bone, or tendon are not visible.
- Stage IV: Stage IV is an injury that is present in muscle, bones, or tendons, which is also exposed in the wound bed. Full-thickness pressure ulcers are deeper and will heal from scar tissue formation. The underlying tissues will be unable to regenerate, and these types of ulcers receive the most attention from attorneys and their LNC, as the damages are significant.
What Else Needs To Be Kept in Mind?
Expert witnesses that are evaluating your pressure ulcer cases will consider the following:
- If scarring is on the patient’s body, it must come from a Stage III or IV pressure ulcer.
- Documentation that stated that the wound is a Stage III and muscle is documented and assessed in the wound bed is simply an inaccurate assessment. That description falls more in line with a Stage IV pressure ulcer.
- If prior documentation stated that your Stage IV is now healing and can classify as a Stage II, not only is this inappropriate staging, but a full thickness wound is incapable of becoming a partial thickness wound.
- Eschar and slough (types of dead tissue) can only form in the thickness wounds, not in partial thickness wounds. If the wound was a Stage II and a slough or eschar was present, it was incorrectly classified with the Stage II designation.
- Deep Tissue Injury (DTI) and Unstageable pressure ulcers have been considered as additional pressure ulcer stages since 2007 by the NPUAP.
Our Professionals will handle Pressure Ulcer Staging and Documentation
SPLNC & Associates, LLC will provide the services of our legal nurse consultants to legal teams that need the reinforcement of an expert witness. If you want to have a better chance of getting your client who was wronged, what they deserve, contact us today!